The people of Louisiana received a critical ruling (3/31/2021) regarding the unconstitutionality of medical care in Angola, the state’s largest prison, where over 6,000 men are held. Among these incarcerated people are many of the oldest and most debilitated, several thousand are sentenced to, realistically, die in custody. They include people previously sentenced as children to the (now unconstitutional) mandatory ‘Juvenile Life Without Parole,’ as well as several thousand who have been sentenced under non-unanimous jury convictions. The latter group, if they had been on direct appeal, would have had their convictions vacated, as a non-unanimous jury conviction has been ruled unconstitutional. They await the U.S. Supreme Court’s ruling on whether an unconstitutional verdict will stand.
The federal court for the Middle District of Louisiana ruled in Lewis v. Cain that Angola’s health care system violates the Eighth Amendment prohibition against cruel and unusual punishment, as well as the Americans with Disabilities Act (ADA) and the Rehabilitation Act (RA). This class action, represented by Promise of Justice Initiative (PJI), looked into a “discovery period” of care from 2015 to 2016. Judge Shelly Dick, supported in process by Magistrate Richard Bourgeois, could not turn away from so many uncontroverted facts presented by the class of patients.
Louisiana’s state penitentiary violated patient’s rights in the following manner, by failing to provide adequate1:
- Clinical care, particularly:
- lack of routine medical equipment in exam rooms;
- lack of adequate medical records management;
- lack of clinical hygiene and spacing;
- episodic treatment of complaints;
- Medical care with qualified providers at sick call;
- Specialty care in a timely manner;
- failure to schedule and track specialty appointments;
- failure to comply with testing and diagnostic requirements;
- failure to execute appropriate follow-up care as ordered by specialist;
- failure to coordinate care;
- Emergency care evaluation by qualified providers and
- failing to timely treat and/or transport to hospital;
- Adequate, qualified staff in infirmary/inpatient care;
- Medical leadership and organization in the following particulars:
- lack of meaningful mortality review;
- use of correctional personnel to manage medical decisions;
- lack of medical staff involvement in budgeting;
- lack of medical supervision by Dr. Lavespere; and
- failure to maintain proper credentialing records;
- Failing to comply with the ADA and RA in:
- Not providing disabled inmates access to programs and services;
- Lacking adequately trained, staffed, and safe orderly assistance where physical modifications have not been made;
- Lacking proper oversight of health care orderlies;
- Not following LSP’s own ADA Directives in maintaining a qualified ADA Coordinator and advisory committee;
- Not integrating disabled inmates within the spirit of the ADA;
- Not training medical staff regarding ADA compliance;
- Failing to evaluate, address, and track ADA accommodation requests;
- Not accommodating disabled inmates in applying discipline;
- Maintaining blanket exclusionary policies for disabled inmates regarding access to various services, activities, and programs
The Angola medical care situation is especially egregious considering that, for the most part, these same allegations came up three decades ago. Prison officials lost in court, and were given specific oversight on developing a constitutionally compliant health care system. They did not. In reading the recent 124-page ruling, it is difficult to see what, if anything, the prison officials improved upon.
Overview of the System
According to the Court, “LSP lacks the infrastructure necessary to provide a constitutionally adequate health care system for patients with serious medical needs. This includes a lack of adequate organizational structure, credentialing and peer review process, health care policies and procedures, clinic space, and a quality control program.” The Court further finds that “overwhelming deficiencies in the medical leadership and administration of health care at LSP contributes to these constitutional violations.”2
It is unclear if the Board of Medical Examiners takes any responsibility for authorizing people on suspended licenses to have absolute control over such a large population of vulnerable patients.
In summary, patients who are suffering some symptoms (whether brutally painful, visibly frightening, or obvious concerns “about a lump”) currently put in a request to be seen by a doctor. They likely need to put this request in several times before being called to sick call, where they are seen by a prison guard who has been trained as an EMT. This sort of training may be good for choking on food, putting pressure on a wound, or a field splint on broken bones, but they have absolutely no training for diagnostic assessments.
A patient, when seen, is in an “exam room” with no diagnostic equipment, and there is no patient chart to track symptoms, chronic conditions, past surgeries, or any medical history. A patient may have had previous orders for testing, but they are often not taken out to a facility where that test can happen. When it does happen, the results are often not forwarded to the right place, and orders from a specialist are not followed by the prison doctors.
Patients often have to re-file a request and, without a chart, are sometimes ordered to undergo the same test from months before. And the cycle continues. Basically, the prison often delays diagnostics as long as possible, does not follow next steps that have been medically ordered, and delays or interrupts treatment on a regular basis.
People are dying because of this cycle, and doing so under a medical team that lacks proper credentials. Angola’s doctors also refuse to do reviews after a patient dies (“mortality review”) and has a complete absence of peer review. This ensures that they do not learn any lessons from a single death, and make zero changes after losing a patient. This is intentional, and quite clear when reading the decision and the uncontested evidence.
For people who have a diagnosed chronic disease, or a physical disability, it does not get much better. These are people who often require a continuum of care, and the primary supporters are fellow incarcerated men trained as “orderlies.” There is a clear lack of oversight of the program, allowing for a great deal of neglect or abuse, on top of the reality that the orderlies are overwhelmed with far too many patients to support.
Disabled people, be they in a wheelchair, deaf, blind, or otherwise less-able: routinely face a “blanket denial” of work and programs, including access to making crafts for sale at the infamous Angola Rodeo. Rather than following the ADA’s basic premise that a public entity will help make things accessible for disabled people (an “accommodation,” like a wheelchair ramp, or subtitles), Angola forces people to file a grievance asking that they be allowed to participate.
Few things can illustrate the scope of the problem better than the prison’s own ADA Coordinator not having any special training, nor records, nor specific duties, and the prison’s own ADA Advisory Committee having zero members. To have things in name only is why oversight boards and commissions need to look under the hood, and to see what is happening in practice.
Staffing and Leadership – Willful Indiffernce, Wanton Disregard, and Knowledge
The Medical Department is managed by an assistant warden; the Deputy Warden, a layperson with no medical training, is the health authority.3
Angola has five doctors and one nurse practitioner. Each doctor was disciplined by the Louisiana State Board of Medical Examiners prior to getting a job at the prison, and all had a restricted license (some have since completed the Board’s requirements and probationary period).4 Although the lawsuit does not say, it is known that doctors have been disciplined for abuse of their patients and abuse of prescription medications. Experts at the trial could not determine if providers were practicing within their credentials because Angola, despite national standards, does not keep credentials on file.5
Correctional officers administer medications, and most of the emergency medical technicians (EMTs) on staff are former correctional officers who increased their pay grade with a low-level training and change in uniform. EMTs handle sick call, where they screen requests to see the doctor.
Orderlies are incarcerated people who have received some training (which ironically they are overwhelmingly barred from using on the Outside). The orderlies provide both assisted living supports and as nursing assistants in the infirmary. They are supervised by security staff, not by nurses, and Angola does not follow their own internal policies regarding the use of orderlies.6
ADA coordinators receive no formal training, nor any additional duties.7
The Court finds the leadership and organizational deficiencies show “deliberate indifference.” This means, essentially, someone chooses not to care. The lack of meaningful mortality review, what a proper medical care provider does to prevent future deaths, ensures that the administration finds no problems in their system. This willful ignorance is in the context where “the death rate nearly doubled from 361 deaths in 2001 to nearly 600 deaths in 2008.”8
There is no annual review of physicians, and no major event reviews. The only thing bordering on review has happened three times since 2010, when the medical director reviews 15 records.
The Court found that the prison administration and medical providers had knowledge of the unconstitutional practices, particularly as this is essentially the same investigation and litigation from 1989 – 1992. At that time, the DOJ investigated and issued a letter of findings which could have been re-dated two decades later. A 1994 trial resulted in a 1998 settlement calling for specific improvements that simply did not happen.9
Deliberate indifference and wanton disregard for human life is not only a matter of failing to correct flaws in health care delivery. Former medical director Dr. Singh recommended to DOC Director James LeBlanc that they not “dig too deep: in investigating a death because “liability is still ours.” Dr. Vassallo testified on how frequently death summaries “misrepresented the facts of the patient’s death.”10
Facilities
To provide care for over 6000 people, Angola has two infirmaries in the “hospital.” Infirmary 1 (“Ward 1”) is for outpatient urgent care, with 20 beds. Infirmary 2 (“Ward 2”) is chronic care for people who require long-term housing (20 beds). Additionally, there are two more dormitories, Ash 2 and Walker 2 (43 beds each) that also serve in this capacity, in addition to the Hospice Ward where people can receive end-of-care medications.11
Ward 2 is managed by a nurse practitioner who oversees over 1000 patients, and only about 100 of the patients are living in what would be considered the informal medical wings of the prison. The rest are spread across general population. According standards in Correctional Health Care, every patient should be within sight and sound of a nurse.12
For context, there are over 5,000 registered hospitals in America, and they are classified into three basic sizes: Small (fewer than 100 beds), Medium (100-499), and Large (over 500 beds).
Within the hospital ward are individual rooms with locking doors and no call system, where Patient K.P., a quadripalegic with a tracheotomy, has been locked facing away from the door with no means to summon assistance.13
Patient #39 was immunosuppressed with a history of congestive heart failure and diabetes. This 65-year old was seen by EMTs seven times in a month. He entered the infirmary with a fever of 103.6 and altered state. The next day, a nurse reported he was masturbating and put him in a locked room with the “hatch up,” and no doctor visited him for three days. On the fourth day he was sent back to general population. Two days later he was laying on the floor vomiting. Angola’s medical director, Dr. Randy Lavespere, along with Dr. McMurdo, ordered EMTs to “not transport” Patient #39 to the hospital. The next day he died.14
Dr. Lavespere, formerly incarcerated himself due to abuses in his practice and hired by the DOC on a restricted license, was promoted to be the DOC’s statewide medical director in 2020.
Patient #18 complained repeatedly for months before being admitted to the infirmary with pneumonia, 55-pound weight loss, and life-threatening vitals. He tested positive for HIV. He was monitored only once daily, and medications, started four days later, were irregularly administered. Within a week his fever spiked and he was transferred to the hospital. A month later he died.15
Clinical Care
Angola’s EMTs hold sick call in the dorms, without patient records, standard medical equipment, or supplies.16 The five physicians do not clinically supervise the EMTs, despite both prison policy and the medical Standard of Care.17Exam rooms were not designed as such, and resemble more like a store room or break room. There is nowhere to wash hands, no privacy, and no paper to cover the exam table. There is not even a blood pressure cuff nor other typical equipment.18 These EMTs are allowed to triage patients and evaluate health requests without having spent a single day in medical or nursing school.
Physicians routinely fail to identify patient diseases, fail to obtain adequate medical history, do not perform meaningful physical examinations, fail to read and monitor testing, and fail to monitor and manage medications.19
Patient #11, having Crohn’s disease, received a colonoscopy six months after the referral. He saw the referred gastroenterologist three months after that. The delay in treatment resulted in five surgeries and two hospitalizations. He was treated by surgeons for two years prior to being managed by a specialist, and prison doctors gave him the wrong dose of a medication that likely resulted in more episodes of fistula.20
Patient #13, having vascular disease and at risk of stroke, was not given the required Statin drugs except for a short 4-month span. He had a preventable heart attack, was hospitalized, and a specialist ordered an echocardiogram test (which took nearly two months to complete). The results never made it in the patient file, and another ECG was ordered during the time Patient #13 had to more hospitalizations for heart failure. Several months later, when he had an episode which indicated a stroke, it took three months to receive a CT scan, revealing a stroke.21
The record indicates what Angola patients know: people presenting with stroke symptoms (slurred speech, for one), have been charged with “intoxication” instead of getting treatment.
Specialty Care
Despite the many failures in the penitentiary health care, it is impossible to avoid the bulk of diagnoses when people are held at Angola for decades. Putting aside whether incarcerated people are more or less likely to contract a specific disease or encounter a specific injury, Angola has an aging population that is no less human than everyone else. Hearts, lungs, kidneys, brains and other vital organs run into difficulty- including things that are preventable or treatable.
Patient #5 complained for two years of weight loss and abdominal pain, to the point where he couldn’t walk, was vomiting and had diarrhea. When he was seen for a bowel obstruction, nobody evaluated the x-ray. Finally, after multiple times he “required hospitalization” over several weeks’ time, he was hospitalized and diagnosed with advanced colon cancer. He died during surgery.22
Patient #17 was at Angola for six years and had chemotherapy for leukemia. A suspicious lung nodule was identified on a CT scan, and two specialists (oncology and pulmonology) recommended follow-up testing. The prison, with full control over Patient 17’s options, did not follow-up. Over the next six months, he could no longer walk and was given a wheelchair. Finally, he was diagnosed with metastasized cancer and died within three months. He was 46 years old.23
Patient #13 was hospitalized for a heart attack, and a vascular specialist recommended a CT angiogram. The test was not done for 10 months. A month later, he had another heart attack, and a month after that he saw a cardiologist, who ordered an echocardiogram. The test occurred a few weeks later, but it was not put in the chart. Over the next three appointments with the cardiologist, they were not able to review the findings.24
Patient #7 received an x-ray revealing a potential malignancy on his lung, at age 58. Three months later he received a CT scan and was referred to a pulmonologist, which took four months: nearly eight months after the initial x-ray. The specialist recommended a biopsy, and Patient #7 did not see the prison doctor for another month, and according to the court records, it seems “the doctor wasn’t sure what the pulmonologist recommended.” A year after the initial x-ray, the pulmonologist saw this patient again, and noted “the biopsy did not occur, what gives?” They recommended a biopsy (again) and “strongly suggest immediate IR [interventional radiology], FNA [fine needle aspiration] of left upper lobe nodule. A month later, still with no biopsy, he had surgery to remove a portion of his lung infested with cancer. After being sent back to Angola, he was scheduled to begin chemotherapy a month later. Two months went by without chemo. Patient #7 put in repeated requests complaining of swelling in his tongue and mouth, and vomiting. An EMT treated the medical complaints with coal tablets and cough syrup. Patient #7 never got chemo. He died.25
Patient #6 was evaluated by a cardiologist for hypertension and significant cardiac arrhythmia, who ordered an echocardiogram and an event recorder test. Only one test was performed, and he was not treated with the proper anticoagulation. Two years later he was hospitalized and anticoagulated. Back at Angola, he was not given the recommended treatment for 10 days, despite developing critical symptoms within four days. He was sent to the infirmary rather than the hospital, and given no diagnostic testing. After four days in the infirmary, he finally received anticoagulation. He died.26
Patient #10 got lab results revealing potentially life-threatening obstructive jaundice. His CT scan revealed a mass in his pancreas, yet was kept in the infirmary (developing a fever) rather than being sent out for a biopsy. After his ultimate diagnosis of pancreatic cancer, he was returned to the Angola infirmary where no coordination occurred with his oncologist. They did not review or monitor his care, and was placed back in general population. Eventually, Patient #10 developed hypotension and an altered mental status and refused care. Finally, he was brought to the hospital, and died in the emergency room.27
Patient O.B. fed himself for three years through a tube and could barely speak due to facial injuries. Despite recommendations from dental providers for reconstructive surgery, Angola’s doctor would not approve because it was considered a “cosmetic surgery.” As of this trial, he still had not received surgery.
Several other patients in the record were documented as having sought treatment for over a year, having waited months to get a test despite multiple requests reporting obvious symptoms, and then receiving a follow-up appointment a month beyond the test being completed.28
Procedures – Sick Call, Referrals, Malingering, and Orders
EMTs enter the dorms to review Health Service Requests, and rarely consult a doctor. From their reviews, less than half of people attending sick call are referred to a provider. Over half of HSRs are, essentially, denied.29 EMTs are supervised by security, not by doctors.30
Having no medical records on hand, requests often receive the same response or same treatment (e.g. aspirin) that did not work.
Sick Call costs $3 while medical emergencies cost $6. This will be debited from one’s account whether or not they received treatment or, in the case of a workplace injury, after being transported to the infirmary. Most incarcerated people at Angola who work receive roughly $1 per day. Additionally, medication costs people $2 to start a new prescription. With access to health care costing between two days and a week’s pay, this is the equivalent of free Americans, such as prison guards, paying anywhere between $250 – $1000 for a co-pay.
“Malingering” is punitive violation that patients can be booked for if it is determined, by security staff, that someone is only seeking sick call so they can get out of work. In Louisiana, people are still sentenced to “hard labor” at the penitentiary, itself originally built as a plantation. Attorneys in Lewis v. Cain failed to produce enough evidence to prove the policy is in some manner unconstitutional, the state’s medical expert agreed the policy should be discontinued.31It isn’t clear if the discipline records throughout the institution were examined, but incarcerated people have a different view than the Court.
Overall, the Court found that having a medical system controlled by security, rather than qualified health care providers, is unconstitutional.32
Patient #20 complained of abdominal pain to the EMTs for over four months. He was never referred to care, and finally the burning pain, weight loss, and vomiting blood resulted in him being admitted to the nursing unit. He died the next day.33
Patient S.H. repeatedly complained for two years of consistent and worsening symptoms, including weight loss and testicular swelling. Eventually he was given testing, revealing renal cancer. S.H. has since died.
Patient Joseph Lewis (top-named plaintiff of Lewis v. Cain) complained to EMTs for 33 months of symptoms consistent with laryngeal cancer. Finally, he received that testing and diagnosis. His case shows repeated “no transport” orders, creating diagnostic and treatment delays. Mr. Lewis has since died.34
Patient #39 was 65 years old, with a history of diabetes, severe coronary artery disease and heart failure. He saw EMTs seven time in a month, with symptoms that included a fever, “breathing but unresponsive,” and “lying on the floor of his cell vomiting and won’t move.” Angola gave “no transport” order three times. After the third, he died.35
Patient #34 complained of flank pain and received an order for an x-ray. A second doctor saw him the next day and noted no explanation for the pain. Three days later, Dr. Lavespere gave a “no transport” order. The next day he died.36The prison does not conduct post-mortem analysis.
Emergency Care
Angola lacks an actual emergency room, despite being a place where over 7000 people are living and working, and instead transports people from the remote location to an ER. The area known as an Acute Treatment Unit (ATU), or “outpatient” facility, sees as many as 76 patients per day despite lacking appropriate equipment. The EMTs, rather than focusing on “emergency” interventions, provide ongoing treatment instead.
People are dying while under this extended care of EMTs, rather than being immediately transferred to a proper medical facility. Patient #1 died in the ATU while being managed by EMTs, as did Patient #15 who was put in and out of the ATU while suffering acute coronary syndrome. Patient #20 also died, while it seemed he suffered internal bleeding. Patient #38, with a history of strokes, died while suffering a stroke.37
Not receiving emergency treatment in time results in preventable effects, and a clear pattern for people suffering strokes not getting treatment within the medically standard 4.5 hour treatment window. Whereas it is a one-hour drive to the actual ER in Baton Rouge, prison security must make a prompt decision to seek proper medical care. Several examples were presented in the litigation that indicate this is a systemic problem.38
Making matters worse, patients who present with “altered mental status” are routinely treated as though they are on narcotics. Even without any clinical indication of illegal drug use, these patients are treated with Narcan (for opioid overdose), given urinalysis for illegal drug use, “often by catheterization,” and stomach-pumping. Through this practice, Patient #37 died, rather than receiving treatment for his seizures.39
Although the plaintiffs presented examples of prison staff seeking to obtain “Do Not Resuscitate” (DNR) orders from patients, the Court did not find it a constitutional violation.
Chronic Care
The Court declined to find the system of chronic care to be unconstitutional, nor to change any prior rulings regarding Hepatitis C care.
Americans with Disabilities Act (ADA)
Throughout the ruling, it is clear that Angola has made very little attempts to be compliant with the ADA, and it is not clear that the staff or leadership have a solid understanding of what the ADA requires of public entities. Some obvious modifications were created since the 1991 standards took effect three decades ago, yet there are 190 architectural barriers that went unrefuted by the Defendants in this trial.40
Medical dorms were designed for unimpaired people, while people in medical wards have been wholesale denied the chance to participate in any classes (including those required to be eligible for release), nor church services, nor other events. This is “unjustified segregation,” in the eyes of the Court, in medical dorms where neither doctors nor nurses make rounds.41
The Court found that the orderly program (using incarcerated people to assist other incarcerated people) “creates an unnecessary risk of harm to disabled and vulnerable inmates.”42 This program is constantly hiring and training new orderlies who are both overwhelmed and underqualified, at times with improper motivations, and the warden admitted “sometimes it is just going to be what it is.”43
Whereas the ADA Coordinator has no added training, and no documentation for reasonable accommodations, there is a wholesale lack of ADA compliance. Exacerbating this is where disciplinary measures do not account for disabilities, such as gassing a blind, mentally ill, man who refused to shave, or using isolated housing where the physically disabled have no manner of calling for help.44
Conclusion
As a matter of law, the Court found that the DOCs medical care in their largest facility is a gross violation of the Eighth Amendment and the ADA. It is clear by the ruling that the current staffing structure cannot simply improve their practices and procedures where it is security staff making unqualified health care decisions that lead to a pattern of preventable deaths.
Read the full decision here.
Proudly powered by WordPress
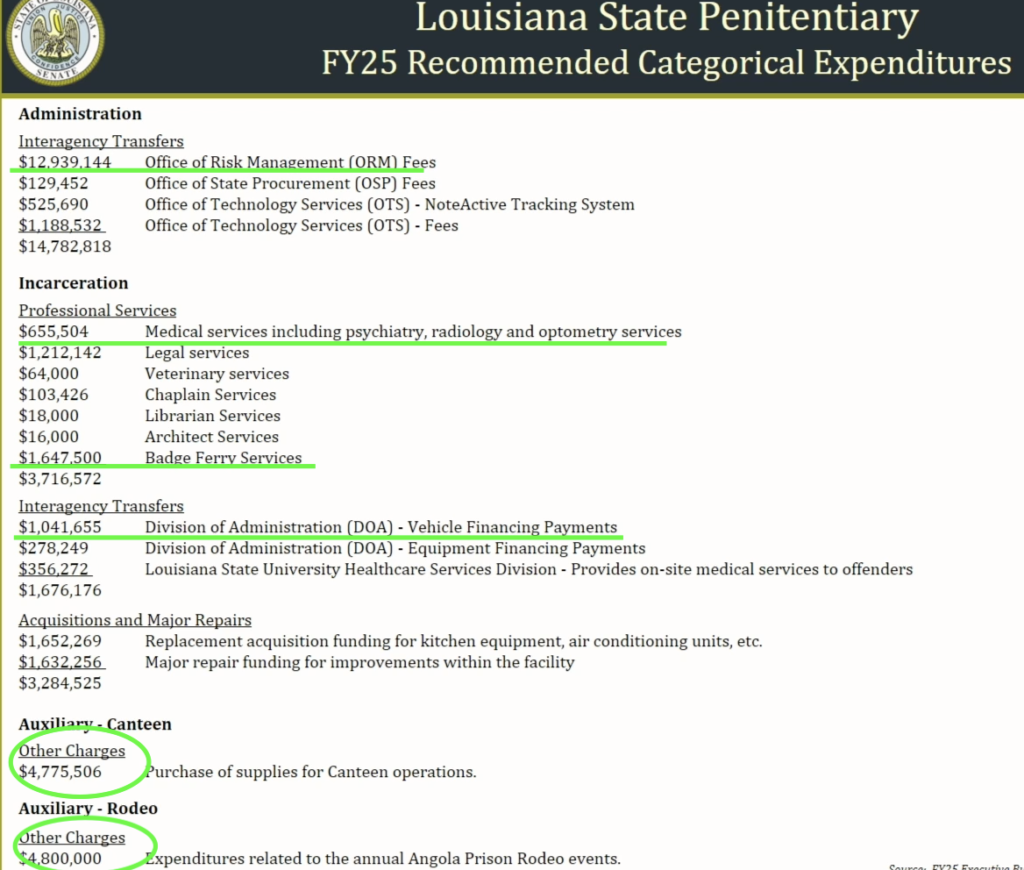
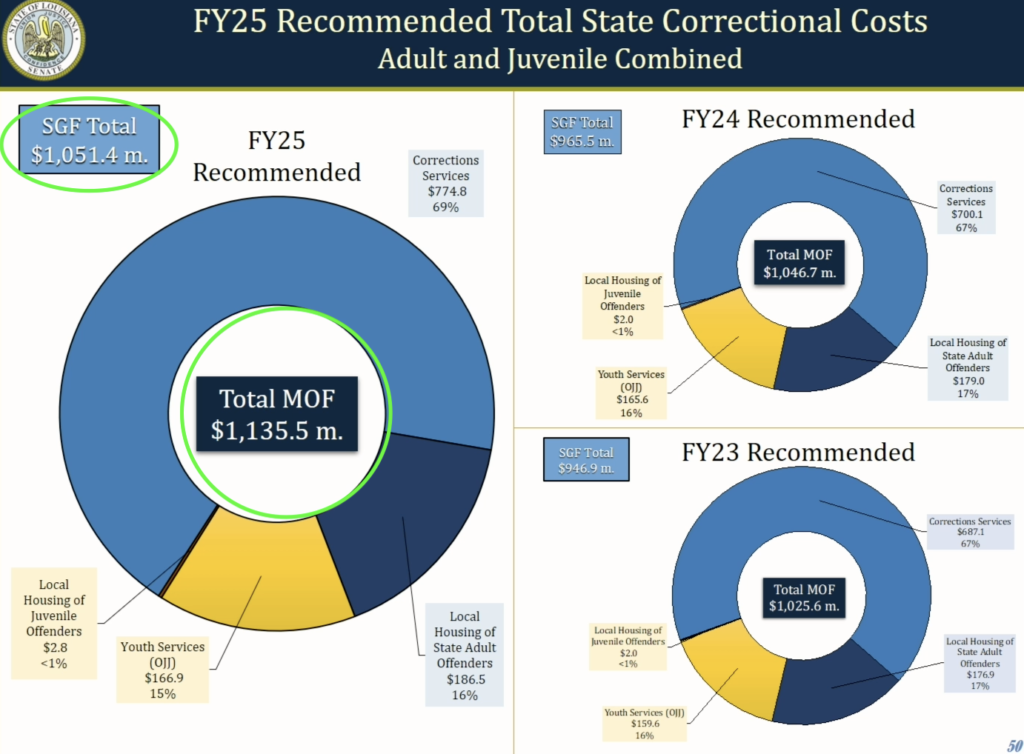
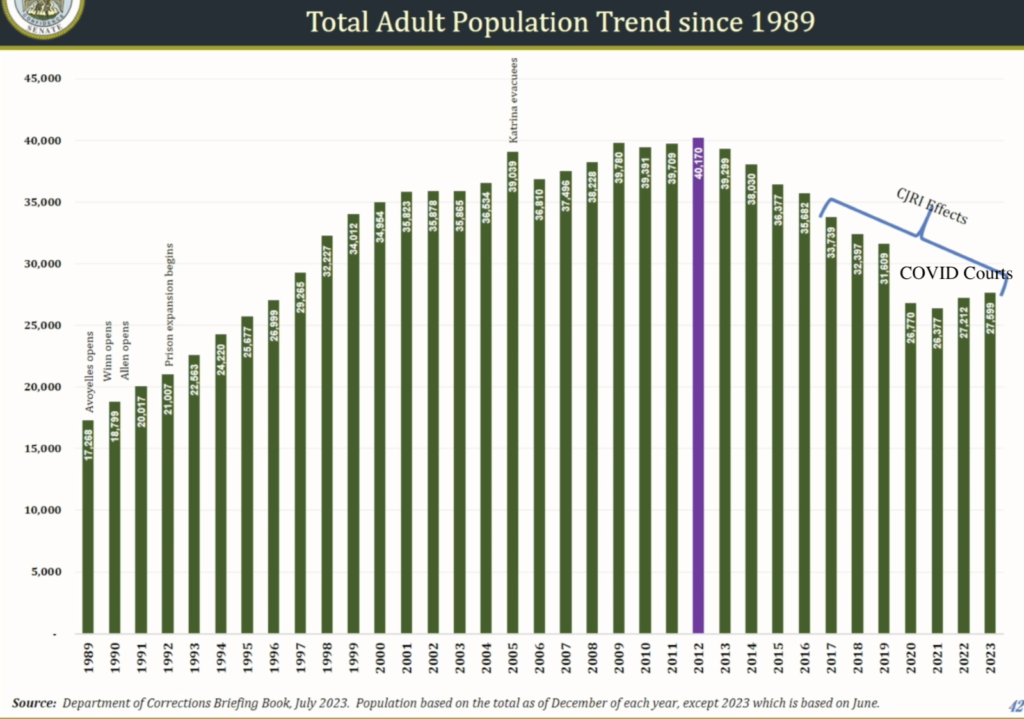
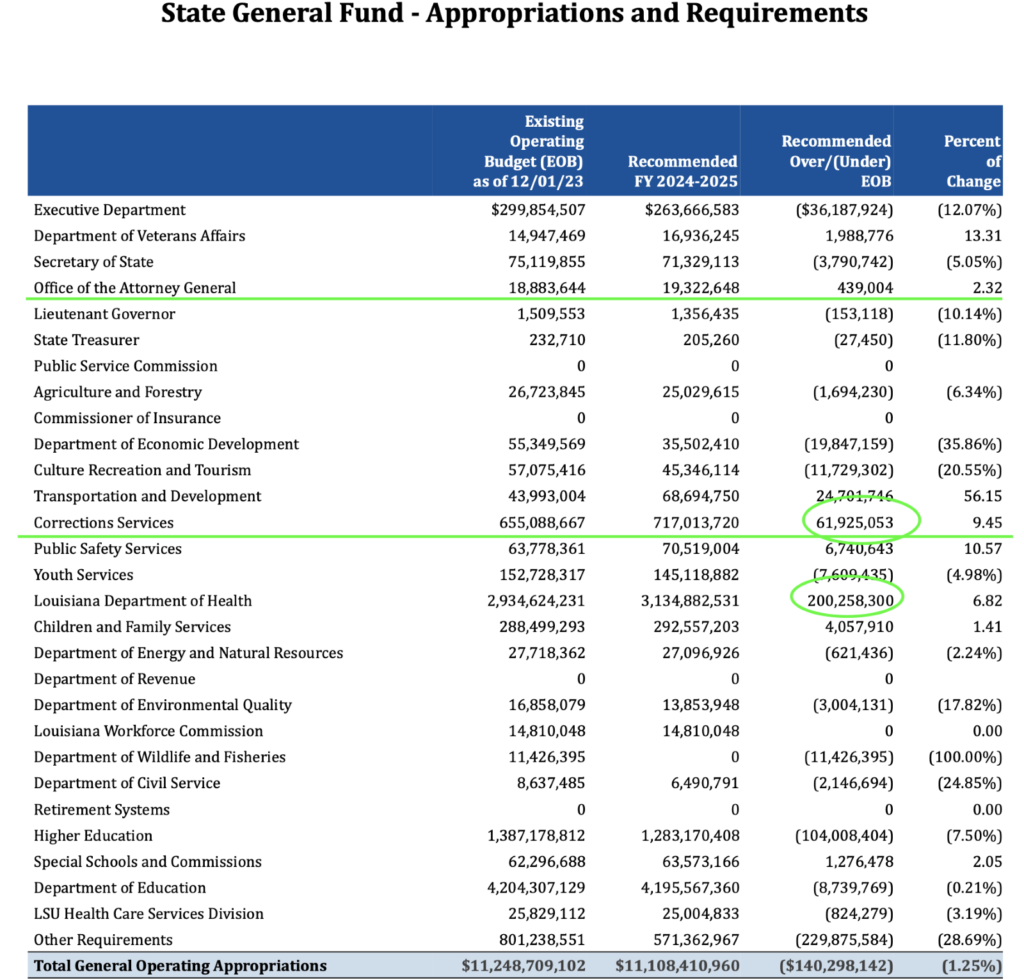
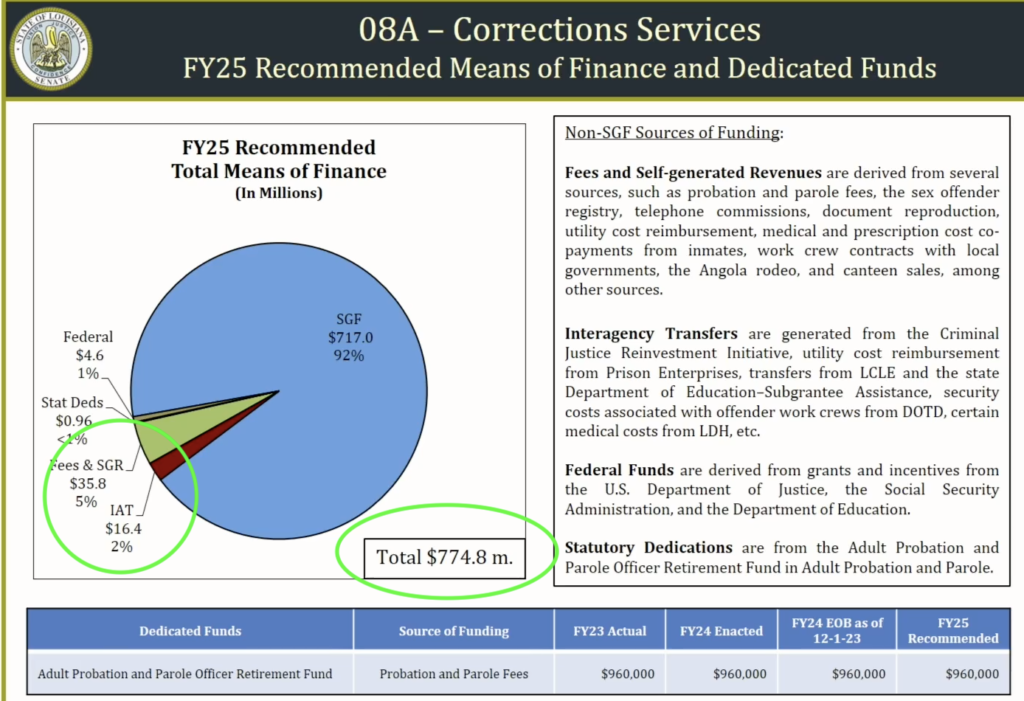

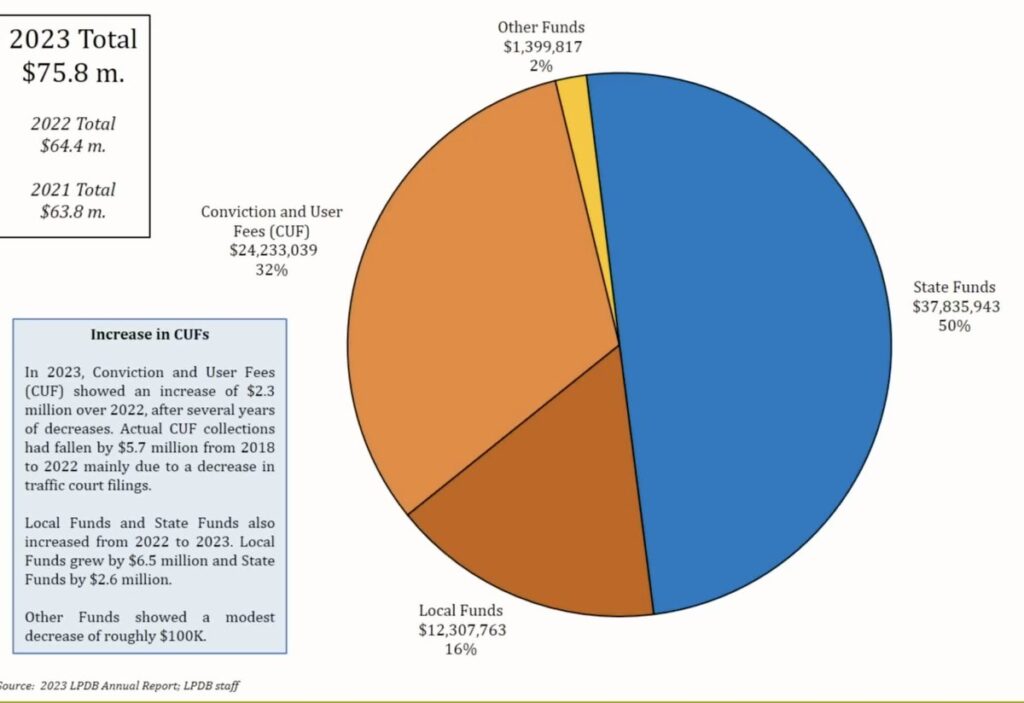
Looking at the overall summary, it is clear that another big piece is keeping the buildings functional, constitutionally compliant, and large enough to handle the influx of people. One shrinking part of the budget is in regard to Winn Correctional Center. In the Feb. 28 budget presentation at the Senate Finance Committee, it was noted that this prison is being leased out to the sheriff in Winn, “for about a million dollars.” It isn’t clear where that million is reflected. DOC Undersecretary Bickham explained to the House Appropriations Committee (March 6, 2024) that there is a Cooperative Endeavor Agreement in place, and the state can take control back from the Sheriff at any time, with roughly six months’ notice.

We are unsure why ICE or Winn Parish Sheriff, who uses LaSalle Corrections to administrate the prison, would want to obscure any details in a contract between two public entities, but it appears that somewhere around $65m is transferred between federal public funds to Winn, according to the Sheriff’s budget report. The entire parish population is only 13,755, and likely includes the number of incarcerated people. It is easy to see why a sheriff’s $14m payroll, pensions, plus local contracts contribute to political influence.
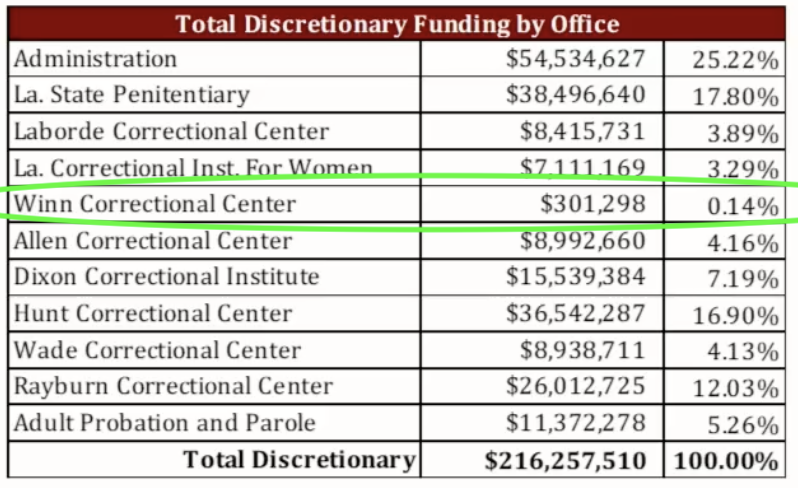
It’s important to understand the relationship between state and local facilities. These parish jails were built in bulk during a time when the state subsidized construction costs and guaranteed the population to be detained. A great summary of this process is in “Prison Capital” (2023) by Lydia Pelot-Hobbes, who was a recent guest on the “From Chains to Change” podcast (listen here).
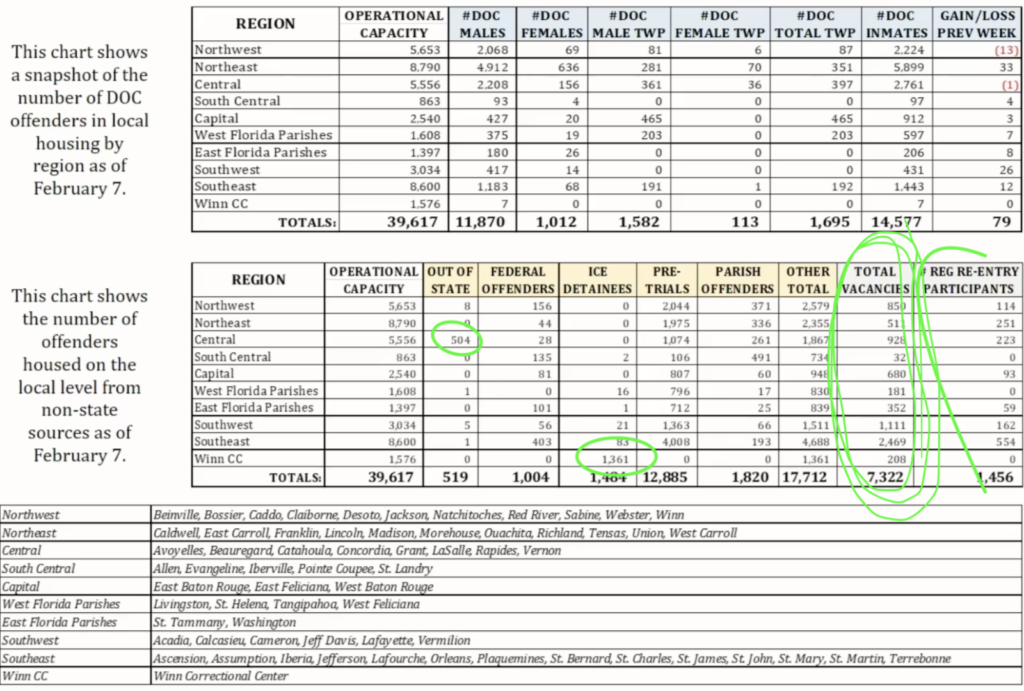
At times, this math does not add up. Rep. Kimberly Coates (D-73) of Tangiapahoa brought up a dilemma in her parish. The local jail is full of state prisoners, for which the sheriff collects the per diem from the state. Meanwhile, there is not enough room for locally arrested people. This forces the parish (not the Sheriff) to pay $800,000 to ship these people out to other jails.
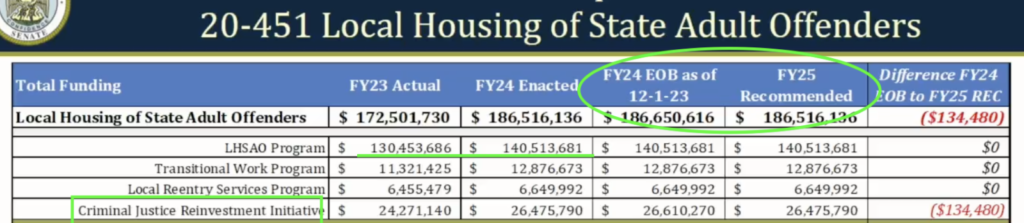
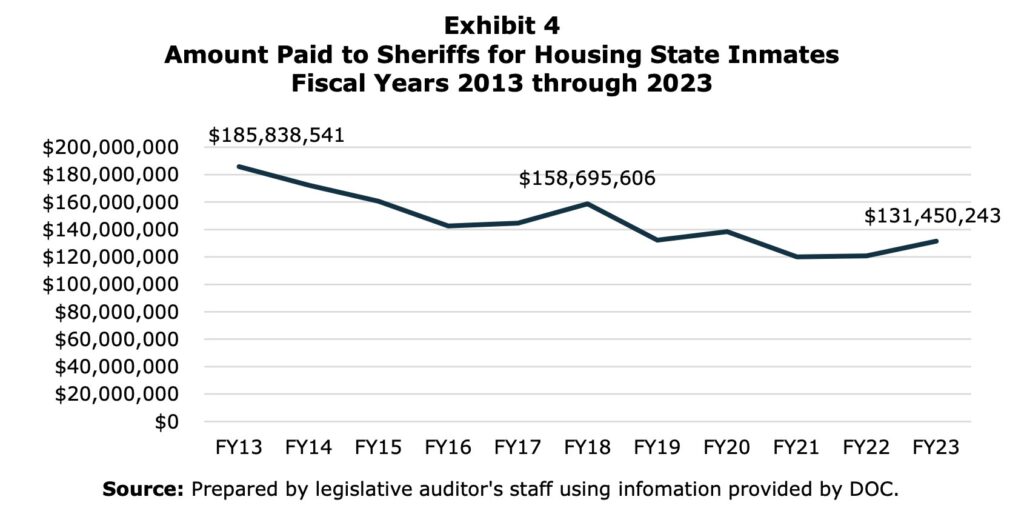
With the state prisons relatively stable in population, unless Winn’s lease is canceled, it is the local jails, run by sheriffs, whose funding was in jeopardy by increasing rehabilitation, decreasing recidivism, providing reentry support, scaling back discrimination, and downsizing prisons. The JRI funding to sheriffs was tailored to garner their support.